
Actor portrayals
Tardive dyskinesia (TD) is a real, chronic condition
It means having body movements you can’t control.
TD is not a side effect. It’s a condition where people experience persistent, uncontrollable movements in different parts of their bodies. These movements can be rapid and jerky or slow and writhing, and they can vary in severity.
Even mild TD movements can make day-to-day activities more challenging and can lead to feelings of worry, frustration, and self-consciousness—which can start to affect your mental well-being.*
*Results based on a survey of 397 people diagnosed with TD (n=173) or suspected of TD (n=224) who were asked, “Tardive dyskinesia may impact you in many different ways. To what extent has tardive dyskinesia impacted you in each of the following areas?” Answers ranged on a scale of 1 (not impacted at all) to 7 (extremely impacted).

Tardive dyskinesia (TD) is a condition in which people taking certain mental health medicines (antipsychotics) over a long period of time experience uncontrollable movements in different parts of their bodies.
Uncontrollable body movements from TD can make it hard to maintain your mental well-being.
Learn more about uncontrollable movements.
SIGN UP FOR INFO
WHAT DOES TARDIVE DYSKINESIA (TD) LOOK LIKE?
TD movements occur in one or more spots of the body and are often seen in the lips, jaw, tongue, and eyes. They can also affect other parts of the body, including the upper body, arms, hands, legs, and feet.
TD can look or feel different from day to day
TD movements may:
- Be rapid and jerky, or slow and writhing
- Occur in a repetitive, continuous, or random pattern
- Present as face twitching, involuntary eye movements, darting tongue, piano fingers, clenched jaw, rocking torso, and gripping feet
- Become worse with stress
Examples of TD Symptoms
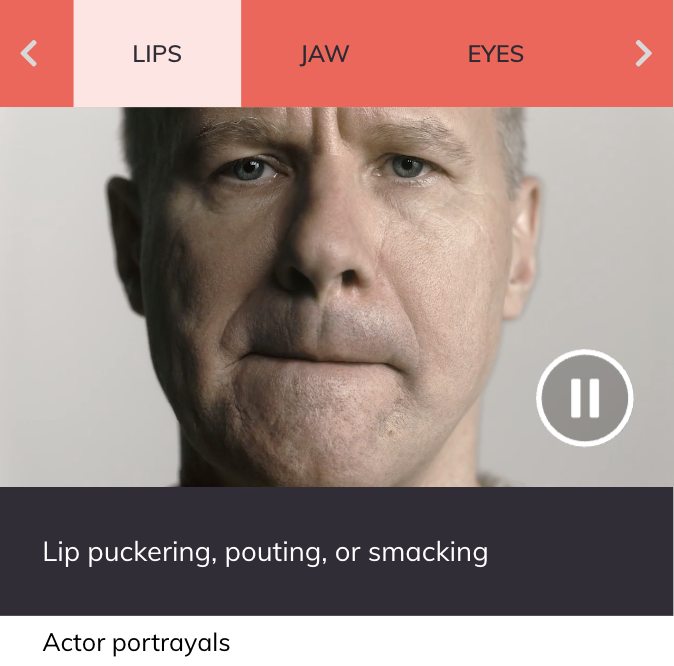
Lip puckering, pouting, or smacking
DO THE ABOVE MOVEMENTS LOOK FAMILIAR?
Now that you have a better understanding of what TD might look like, take this short quiz to see if you or your loved one's uncontrollable movements could be consistent with TD.
Take the symptom checker quiz
1.Do you or your loved one have uncontrollable body movements (such as lip pursing or puckering, darting tongue, excessive blinking, twisting hands, dancing fingers, torso jerking, rocking, twisting, etc)?
This questionnaire was developed by Neurocrine Biosciences. This questionnaire has not been validated and is intended to provide general information about tardive dyskinesia assessment and not medical advice for any particular patient.
What causes shaking hands or uncontrollable shaking of your body or limbs may not be TD. Because there are different kinds of movement disorders, your healthcare provider may ask you to perform a variety of movements or actions to help figure out what movement disorder might be affecting you.
WHAT CAUSES TARDIVE DYSKINESIA (TD)?
Taking certain mental health medicines (antipsychotics) over a long period of time is thought to cause too much dopamine activity in the brain. Dopamine is a chemical in the brain that plays a role in how we move. Too much dopamine activity in the brain could lead to uncontrollable body movements. And those movements may keep controlling your body.
Antipsychotics are prescribed to treat conditions like:
- Depression
- Schizophrenia
- Bipolar disorder
- Schizoaffective disorder
Other medicines used to treat upset stomach, nausea, and vomiting may also cause TD.
Medications that may cause TD
If you are taking or have taken any of the following medications over a long period of time and are experiencing uncontrollable movements, it’s important to share this information with your healthcare provider. Understanding your treatment history can help your healthcare provider determine if your movements may be TD.
First-generation antipsychotics
- Chlorpromazine (THORAZINE)
- Molindone (MOBAN)
- Fluphenazine (PROLIXIN)
- Loxapine (LOXITANE)
- Haloperidol (HALDOL)
- Perphenazine (TRILAFON)
- Thioridazine (MELLARIL)
- Thiothixene (NAVANE)
- Trifluoperazine (STELAZINE)
Second-generation antipsychotics
- Aripiprazole (ABILIFY)
- Asenapine (SAPHRIS)
- Brexpiprazole (REXULTI)
- Cariprazine (VRAYLAR)
- Clozapine (CLOZARIL)
- Iloperidone (FANAPT)
- Lumateperone (CAPLYTA)
- Lurasidone (LATUDA)
- Olanzapine (ZYPREXA)
- Paliperidone (INVEGA)
- Quetiapine (SEROQUEL, SEROQUEL XR)
- Risperidone (RISPERDAL)
- Ziprasidone (GEODON)
Other medicines that may cause TD
- Prochlorperazine (COMPAZINE, COMPRO)
- Promethazine (PHENERGAN, PROMETHEGAN, PHENADOZ)
- Trimethobenzamide (TEBAMIDE, TIGAN)
- Thiethylperazine (TORECAN)
- Metoclopramide (REGLAN)
For educational purposes only. Not intended as an exhaustive list of medications that may cause TD. Be sure to discuss any specific questions or concerns with your healthcare provider.
Third-party trademarks are property of their respective owners.
Do not stop taking your medicines without talking to your healthcare provider.
When can tardive dyskinesia (TD) start?
TD symptoms may start a few months or even years after taking certain mental health medicines (antipsychotics). In some cases, symptoms may not be seen until after the medicines are stopped.
In addition to taking mental health medicine, the following factors may also play a role in your risk for TD:
- Being 55 years of age or older
- Being postmenopausal
- Substance abuse
- Having a mood disorder
Never change or stop taking your medicine without speaking with your healthcare provider.
TD Treatment options are available
Learn about a prescription medicineLooking to take the first step in managing your uncontrollable body movements?
Help may be closer than you think. More than 25,000 neurologists, psychiatrists, and advanced-practice healthcare providers who have experience with diagnosing and treating TD are available.† Use the Find a Specialist tool to take your first step.
†Data on file; 08/2025. Neurocrine Biosciences, Inc.

Within the last year, the Doctor Discussion Guide has been downloaded over 115,000 times,‡ helping many have meaningful discussions with their doctor.
‡Source: Google Analytics 4, January 1, 2025–August 31, 2025.

Get information about td.
Learn more about TD and how to start a conversation with your healthcare provider about TD diagnosis and treatment.
Sign up for Info
Jeff was compensated by Neurocrine Biosciences, Inc. to share his story
“[People] see that I have challenges like schizophrenia and tardive dyskinesia. And they see all that I’m able to do despite these disorders. If I can do it, then other people can do it as well.”
–Jeff
living with schizophrenia
and tardive dyskinesia